
3d Surgical Planning and 3d Printing – Innovative Technology to Correct Hip Instability after Expandable Prosthesis Reconstruction
2Msk Lab, Imperial College London, London, UK
Dislocation is a common complication after proximal and total femur prosthesis reconstruction for primary bone sarcoma patients, mainly in expandable prosthesis. Hip stability forces acts on the hip during the lengthening forcing head of prosthesis laterally, with non-sufficient reported good surgical solutions.
Objective: Assess novel 3D surgical planning technology, in supporting correction of young children suffering from hip instability after expandable prosthesis reconstruction. This innovative technology creates a new dimension of visualization and customization, improving understanding complex problems and facilitate surgical decisions and procedure.
Method: Two children Ewing Sarcoma patients with proximal femur, 3/5 years at diagnosis, treated with conventional chemotherapy, followed by proximal femur resection, reconstructed with expandable prosthesis, with hip migration that developed gradually during 24m lengthening process. Custom 3D planning software allowed surgeons visualize anatomical status and assess osteotomies planes and desired acetabular roof position after hip joint reduction. Plans used to generate 3D printed PSIs (Patient-Specific-Instrument) to guide osteotomies during shelf and triple osteotomy surgeries. PSI planning accuracy verified by comparing cutting planes and post-op position of the acetabulum.
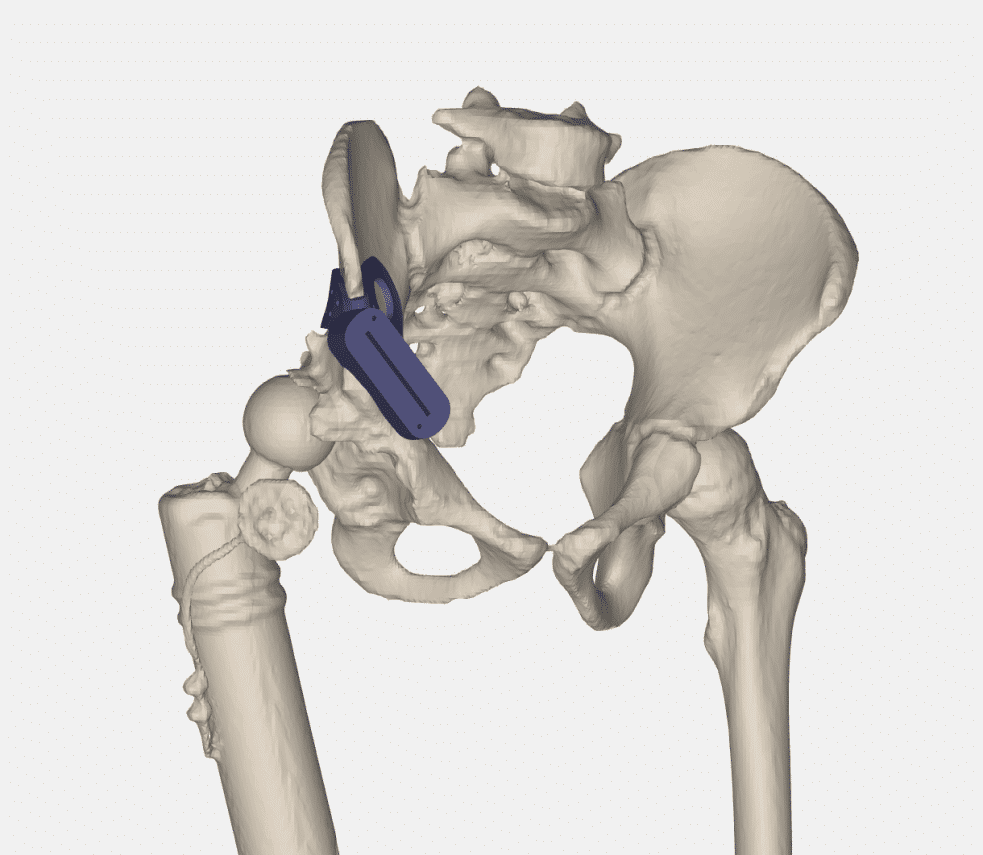
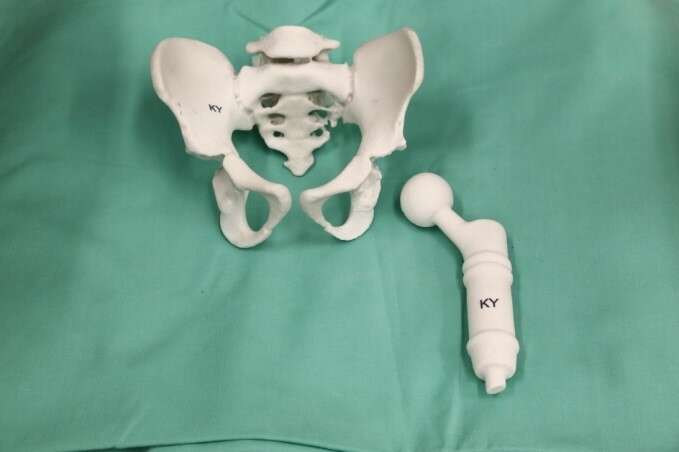
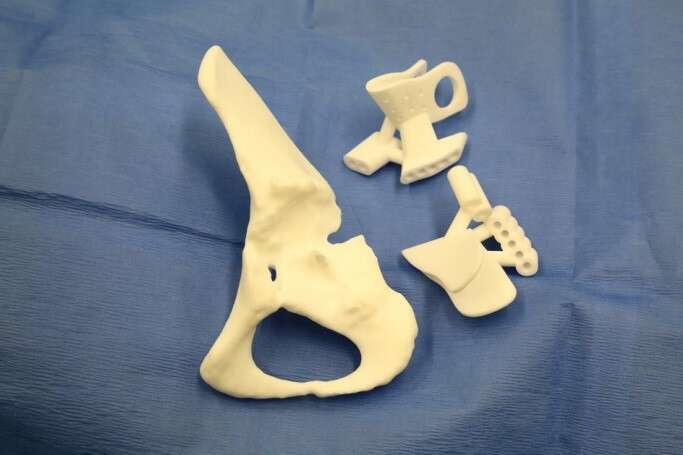
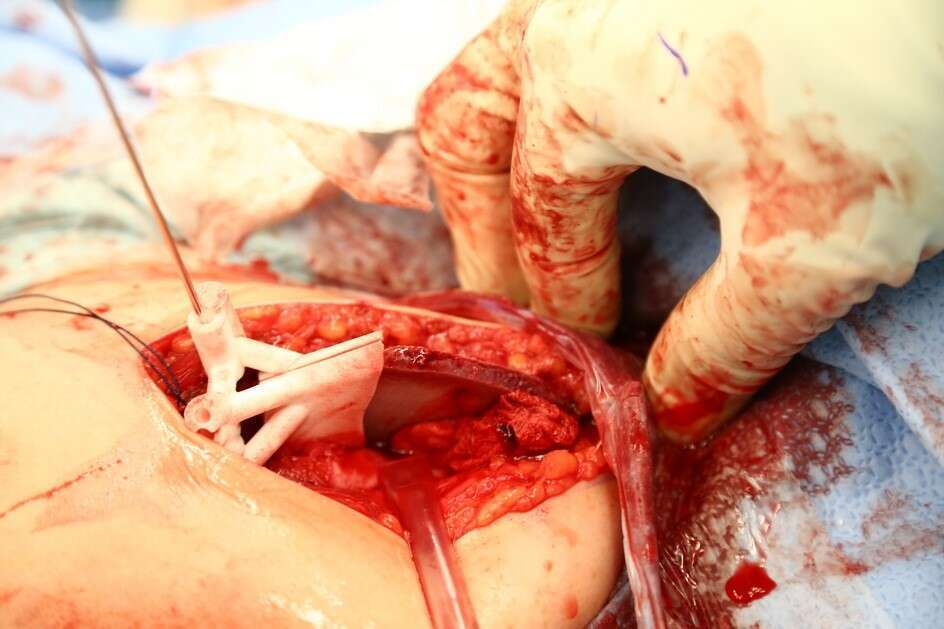
Results: Surgeons reported excellent experience with 3D models, improve understanding of prosthesis head and acetabulum relationship, with a clear view of the osteophytes and bone formation surrounding the pseudoacetabulum, and osteophytes inside the native acetabulum. Good fit and PSIs` simplicity of use reported. Hip stability was good during surgery and in immediate post-op period. X-ray showed good centered position of hip and good levels of the osteotomies.
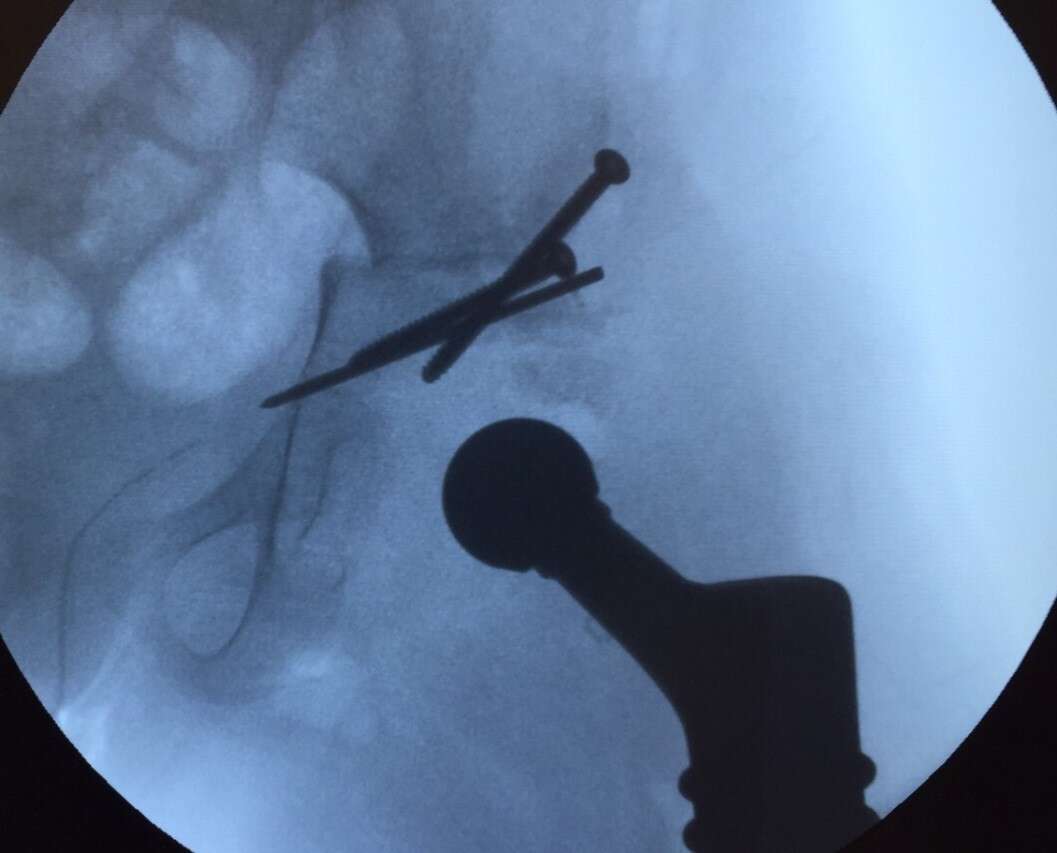
Conclusions: 3D surgical planning and printing was very effective assisting surgeons facing complex problems compared to CT&MRI ability to visualize all bony formation and entrapment of prosthesis in the pseudoacetabulum. Planning and executing surgery with guidance of PSIs allowed improved surgical results, showing 3D technology can improve hip stability in this unique cohort of patients.
Powered by Eventact EMS