
Approach to the Fixation of a Scaphoid Waist Fracture, Perpendicular to the Fracture – Cadaver Model
2Medical Center, Hadassah-Hebrew University, Jerusalem
3Pathumthani, Thammasat University
Objective: The majority of waist fractures of the scaphoid have been found to be horizontal oblique. In these fractures, screw fixation along the longitudinal axis of the scaphoid differs significantly from a screw perpendicular to the fracture and may be less efficient. Our hypothesis was that fixation of a horizontal oblique fracture with a screw perpendicular to the fracture is possible from a volar as well as a dorsal percutaneous approach, in the majority of cases. This approach may differ from the common approaches used today.
Methods: Computed tomography (CT) of 12 cadaver wrists were performed in three positions – maximum flexion, neutral position, and maximum extension. The scans were evaluated using a 3D model, including simulation of transverse (90-degree) and horizontal oblique (60-degree) fractures and of the possible screw axes, examining which approach better enables screw insertion perpendicular and in the center of the fracture.
Results: The preferred approach for perpendicular screw placement in transverse (90-degree) fractures was found to be proximal-dorsal in flexed or neutral positions and distal in the extended position (volar to volar-radial trapezium). For a 60-degree fracture, the best approaches were proximal-dorsal in flexion or distal transtrapezial in the extended or neutral positions (through the radio-volar trapezium). In these approaches, the screw could be placed perfectly perpendicular and in the center of the fracture in all specimens. In extension, for a 60-degree fracture, a distal screw could be placed at a 23-degree angle (SD 8) to the perpendicular axis, at an approach radial to the volar-radial trapezium.
Conclusion: In this simulation of scaphoid waist fractures, including the more common horizontal oblique fractures, a perpendicular screw may be placed in the center of the fractures both dorsally or through a distal transtrapezial approach.
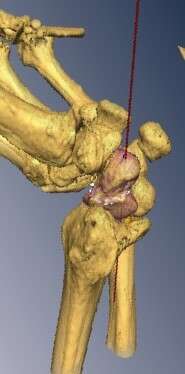
Figure 1
Distal approach to a horizontal oblique fracture of the scaphoid, volar-radial to the trapezium, in wrist extension.
Powered by Eventact EMS