
A Novel Mesenchymal Stem Cell Therapy for Immunomodulation Following Vascularized Composite Allotransolantation in a Rat Forelimb Model
2Sackler Faculty of Medicine, Tel Aviv University
3Orthopaedic Surgery, University of Pennsylvania
4Anatomy and cell biology, University of Pennsylvania
Introduction: Immunosuppression risks are a major concern in the field of vascularized composite allotransplantation (VCA). The research goal of establishing lifelong allotransplant immune tolerance may reduce patient morbidity and lead to expanded VCA indications. Our purpose was to characterize a rat forelimb VCA model, and utilize it to compare the in vivo immunomodulation efficacy of gingival derived mesenchymal stem cells (G-MSCs), bone marrow derived mesenchymal stem cells (BM-MSCs), and rapamycin therapy. We hypothesized that G-MSC treatment would inhibit VCA rejection more efficaciously than BM-MSC.
Methods: Twenty-four Sprague Dawley rats, and seven pairs of Wistar Kyoto (WKY) and Lewis (LEW) rats, were used to establish the forelimb VCA model. Following elucidation of the VCA model, forelimb transplantation was performed on pairs of MHC-incompatible rats(WKY donor, LEW recipient), which were divided into 4 groups including: control(n=5); rapamycin(n=4)(2mg/kg/day via subcutaneous osmotic pump for 28 days postoperatively); BM-MSCs(n=6) or G-MSCs(n=5) in which stem cells were intravenously administered on post-operative days(POD) 0, 3, 7, and 14. First signs of acute rejection, and complete rejection, were monitored. Micro-CT was performed to evaluate for healing at the osteosynthesis site. Statistical analysis was performed using the student t-test and a standard threshold for significance (p<0.05).
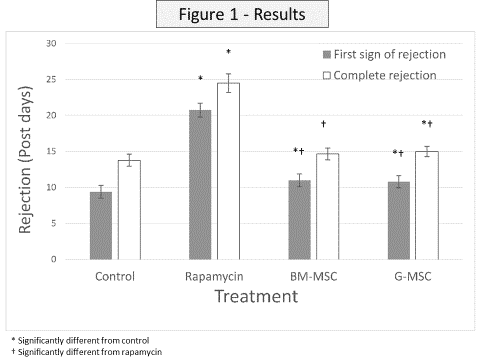
Results: Perioperative rat and limb survival rates were 86.5% and 84%, respectively. Both MSC treatments significantly delayed the onset of acute rejection while only G-MSC delayed the onset of complete VCA rejection over controls, with no differences between MSCs groups (Figure 1). Rapamycin treatment was significantly more effective in delaying allograft rejection in comparison to all other groups. Micro-CT imaging on POD 14 revealed that none of the treatments impaired bone healing.
Conclusions: Forelimb vascularized composite allotransplantation is feasible in the rat model.
Although MSCs show promise for preventing rejection, pharmacotherapy remains the most effective mechanism. Future studies will examine MSC along with rapamycin to see the additive effect.
Powered by Eventact EMS