
Risk, Complexity and Special Health Care Needs Scoring for Hospitalized Children with Medical Complexities(CMC) in an Academic Hospital of Univ California San Francisco, California
High acuity, complexity, & special needs in hospitalized pediatric patients have been shown to have measurable economic costs & effect on quality of care.
This study examines criteria for Children with Medical Complexities (CMC) & scoring tools to stratify risk using Exeter HOMES(Hospitalization, Outpatient care, Medical chronic disorders, Extra services, & Social determinants) complexity index, & a validated Children with Special Health Care Needs (CSHCN) Screener. By measuring both complexity & special needs an effect on higher health care utilization, Length of Stay, (LOS) & readmission rates (RR) are predictive of economic burden.
A 6-month retrospective observational study was conducted from May-Nov, 2018, for a(n=204) pediatric patients, admitted to the general pediatric unit. Demographics, ICD10, PCP’s, total number of admission (TA), Gestational age, LOS, #RR, occurring in last 180 & 90 days of the study period. Criteria fitting CMC & (Cystic Fibrosis, asthma, cardiac, & mental health), Gestational Age (GA), clinical encounters, medications, medical devices, & social determinants were reviewed for CMC patients. The total number of RR, LOS & Risk scores were determined. The scoring was compared for CMC & an equal number of non-CMC pediatric patients admitted during the same study period using Excel Statistical program.


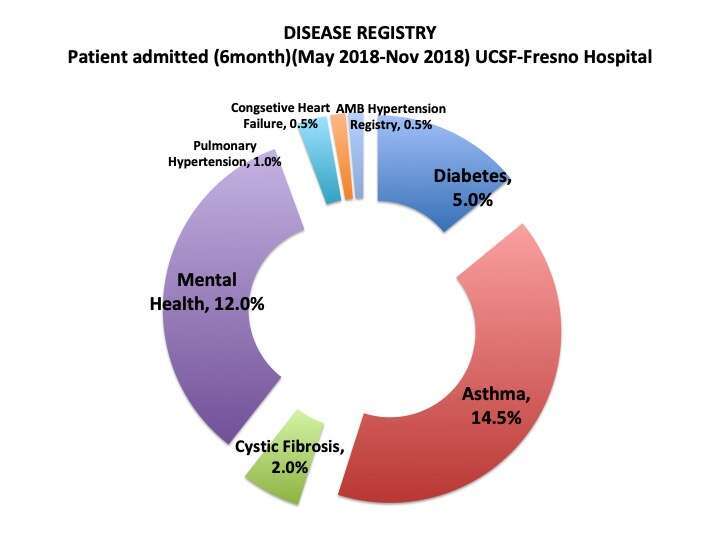
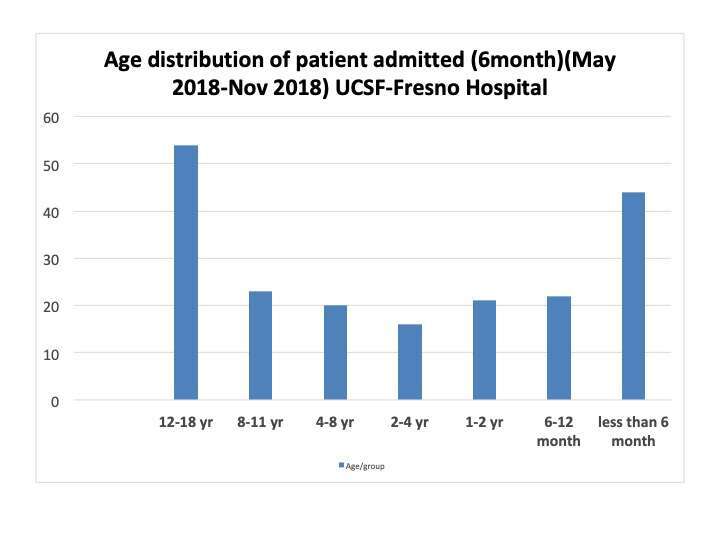


For CMC patients, the complexity index scores are 2.5- 2.6 times higher & LOS also increases by 2.1. Twenty percent of patients of admitted are of high complexity. Validated risk stratification tools applied to CMC patients demonstrate increased LOS & RR that are more than twice that of the non-CMC patients. A high-risk index can lead to inefficient health care utilization, unaccountable patient/family cost, & poor outcomes.
Powered by Eventact EMS